Your week got you feeling like the dog in the “this is fine” cartoon? Trying to pry your eyes away from yet another dumpster fire? We’ve got a few funny and entertaining social media recommendations for you! Don’t worry, that fire will still be raging – but we’ve got to rally strength before we can take down systems that are failing, right?
Continue readingHolidays in the Hospital
No one wants to be in the hospital, ever. But spending the holidays in the hospital is an extra downer, to say the least. Hospitals feel sterile, cold, and impersonal – everything the holidays shouldn’t be. Here’s some tips for making your stay over the holidays feel a little more warm and a touch more comforting.
Continue readingLooking for Help With Clinical Trials?
Finding a clinical trial can be overwhelming. Patients are often left to search for trials on their own, leaving them with more questions than answers. Fortunately, our friends at The Leukemia & Lymphoma Society provide a free service to take this burden off patients and their families!
Continue readingSurvival Is Insufficient
Now there is scientific research showing that the young adult cancer population, aged 18-39, is the most isolated age-group who experiences cancer, and that this isolation is linked to all sorts of quality of life issues. It affects survival rates, reintegration into normal life, and a host of other things. There is data showing that surviving cancer is not enough, we must also be helped to thrive. There is data showing that survival is insufficient.
Continue readingYou Don’t Look Sick: Illness, Pain, and Being Believed
I do not fit the cultural touchstone of a chemo patient. I have not lost my hair from any of my various treatments. I haven’t lost a ton of weight. Sometimes, I desperately wish my appearance would match the war my body was waging on the inside, so others would know the pain I felt.
Continue readingPostcards from the Edge: Medical Phone Calls Edition
Christina’s Guide to Not Losing Your Ever Loving Mind: Making Insurance, Prescription, and Medical Phone Calls
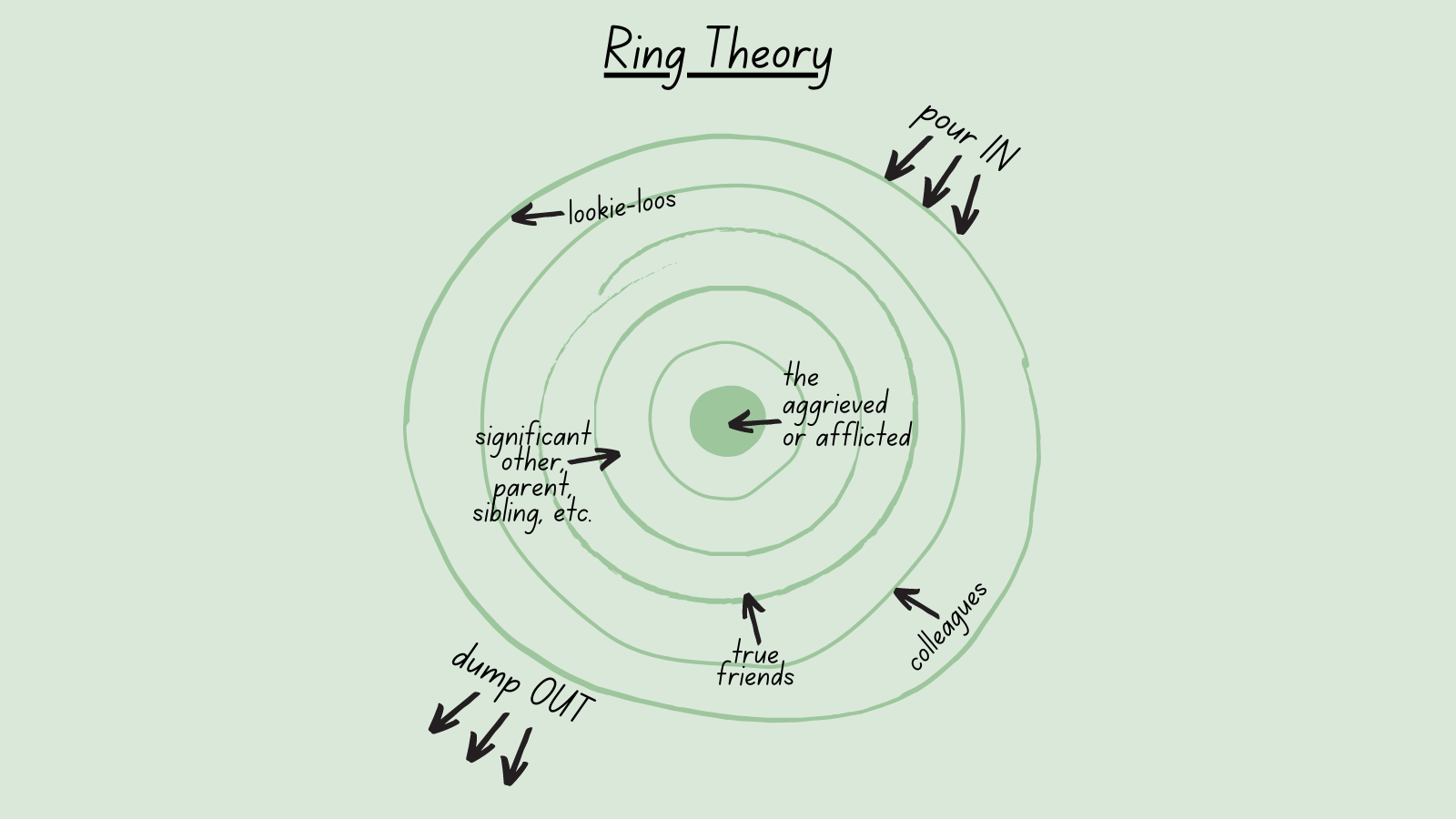
Continue readingRing Theory
Have you heard of Ring Theory? It’s a fairly simple concept of support and communication that can be extremely helpful for cancer patients and their loved ones.
Continue readingWant to Learn How To Take Advantage of Clinical Trials?
Join Patients Rising on May 14 at 1pm ET (10am PT) for an informative webinar on taking advantage of clinical trials. Clinical trials are at the heart of all advances in medicine. They lead to new innovations in preventing, detecting, and treating disease. They allow researchers to test new treatments and new ways to use existing treatments. Clinical trials determine if new treatments are safe and effective.
There are many reasons to participate in a clinical trial. In this webinar, their panel will help you explore the benefits and risks and how clinical trials can fit into your healthcare plan. They will explain why you should care about clinical trials, how they work, and potential risks. They will answer your questions about clinical trials and point you to valuable resources to search for and learn more about clinical trials.
Please join Patients Rising on Tuesday, May 14 at 1pm ET (10am PT)!
Cancer Care by Zip Code: Examining Geographic Health Disparities in the US
ASCO Connection recently published an article talking about health disparities (“a term commonly used to describe differences in incidence, prevalence, mortality, and burden of cancer related to conditions among specific populations, including racial and ethnic minorities, sexual and gender minorities, older adults, and rural patients, among other groups”…that is a mouthful!) based on where someone lived who was diagnosed with cancer. In the world of cancer survivorship, Lacuna Loft sees people from all over the country. We have participants who are based in urban areas but for whom getting to a place for survivorship support is cumbersome all the way to people who live rurally and have no cancer center (or other known young adult cancer survivors) within a hundred miles. This article isn’t based on young adults specifically, but it underlines the effect that geography has on outcomes…on whether people are surviving their cancer.
“Exciting new breakthroughs in cancer research are helping to make great strides in what is possible for patients with cancer. But they are not necessarily leading to equitable disease outcomes.
According to the Centers for Disease Control and Prevention (CDC), while the overall age-adjusted incidence of cancer is lower in rural areas than urban areas, rural areas have higher cancer death rates. This difference in mortality is growing wider over time. In these instances, new cutting-edge therapies are not enough.”
The fact that this research is fairly recent, done within the last few years, also underlines how important it is for patients to speak up. If a physician doesn’t ask you questions but you have something in your cancer treatment regime that is overly burdensome (traveling for treatments for instance), taking charge and using your patient voice to advocate for better care is a must. This is true in the cancer treatment space as well as the cancer survivorship space. Sometimes, a better solution isn’t possible…but we can always ask!
Read more of this very interesting article here.
Yoga Video For Cancer Patients
With the buzz of the holiday season almost upon us, sometimes it’s nice to slow down for a few minutes. With that in mind, today we’re sharing a yoga tutorial specific for cancer patients. With every pose done in bed, and a bit of guided relaxation, this yoga video is sure to relax and invigorate. If you give it a try, let us know! Have you used yoga in your survivorship?